Reorientation in the Era of Covid 19
Covid Update 6/10/20
 Loading...
Loading...
Covid Update 6/4/20
 Loading...
Loading...
Covid Update 5/28/20
 Loading...
Loading...
 Loading...
Loading...
Covid Update 5/21/20
 Loading...
Loading...
Covid Update 5/18/20
 Loading...
Loading...
Covid Update Call - 5/14/20
Covid Update 5/7/20
 Loading...
Loading...
Covid Update 5/4/20
 Loading...
Loading...
Covid Update 4/30/20
 Loading...
Loading...
Covid Update 4/23/20
 Loading...
Loading...
Covid Update 4/16/20
 Loading...
Loading...
N95 Reprocessing - DETAILS
Starting TODAY we are launching N95 Reprocessing! This means your own N95 will be returned to you at the beginning of your shift STERILIZED. We are expecting to use these masks for 4-5 shifts rather than 7. To participate:
Label your N95 on the outside edge of the bottom of your mask (near the gray print) with your name and ANES there are many sharpies in the CCHS office and the Wilmington work room for this purpose. See attached image.
At the end of the day doff your mask into the soiled mask hamper outside the locker room. Hampers are labelled for masks and are in the scrub anteroom at CHS and in M and W locker rooms at Wilmington. PLEASE do not put scrubs in this hamper. Please wash your hands after doffing. Please only doff your masks into these hampers so that they are returned to us (as opposed to HVIS or the MICU).
Masks are returned to the anesthesia office at CCHS and the anesthesia work room at Wilmington. Masks are returned the next day after 9 am so…
If you have two shifts in a row, you will be issued a second N95 mask to alternate for decontamination.
The masks will be marked during each decontamination process and inspected. If you have an N95 that has been labelled with either 4 decontamination labels or a red mark from the decontamination unit, please show it to Theresa/Lisa/Wendy to get a new mask.
Please feel free to reach out to me and Dr. Abdullah if you have any issues. This is all new so hopefully the kinks will work themselves out over the next few days.
Read Siry, MD
Director of Education, Department of Anesthesiology


Covid Update 4/13/20
 Loading...
Loading...
Covid-19 Update 4/9/20
 Loading...
Loading...
Covid -19 Update 4/8/20


Covid update April 6
 Loading...
Loading...
Aerosol Box
For anyone interested, some data showing efficacy of the box in preventing widespread aerosolization during a simulated cough. Done at Boston Medical Center and recently published on the New England Journal website:
https://www.nejm.org/doi/full/10.1056/NEJMc2007589
Jim Leonard
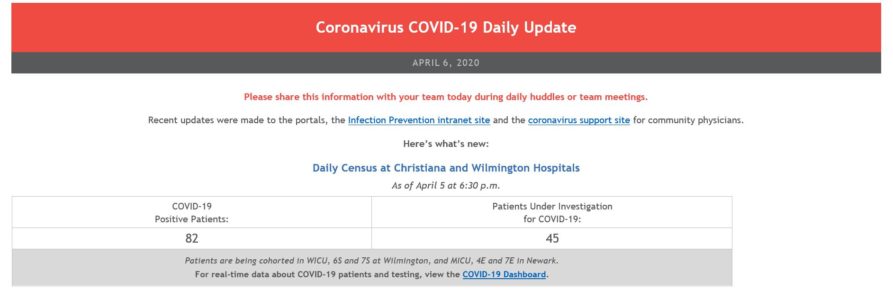
Caregiver Coronavirus Daily Update - April 6, 2020

PROCEDURE CHANGE: HEPA filters and floor intubations
Respiratory has an ample supply of BacT filters (their version of HEPA filters). To conserve our supply of HEPA filters please use the RESPIRATORY BacT filter at floor intubations. The RTs should have them, they are in the MICU and every covid floor, they are available in the ER and in every code cart in the system. Please discuss the location of the filter PRIOR to bringing the HEPA filter from the airway box into a patient room.
Thank you for making lots of quick changes. Please let me know if you have questions
Read
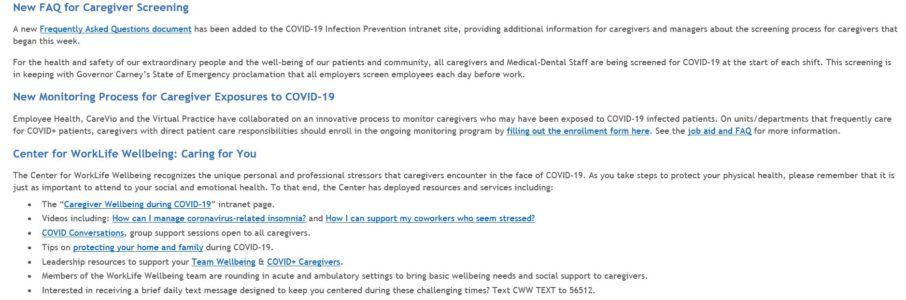
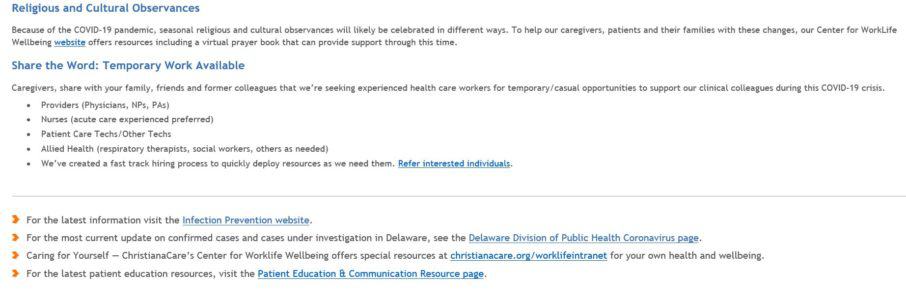
New Caregiver/Medical-Dental Staff Screening to Start Monday, April 6
From: Physician Relations
Sent: Friday, April 3, 2020 4:15 PM
Subject: New Caregiver/Medical-Dental Staff Screening to Start Monday, April 6
Importance: High
Dear Caregivers,
For the health and safety of our extraordinary people and the wellbeing of our patients and community, all caregivers will be screened for COVID-19 at the start of each shift beginning Monday, April 6, at 6:30 a.m. This screening is in keeping with Governor Carney’s State of Emergency proclamation that all employers screen employees each day before work.
Understanding that this is a demand on caregivers’ time, we have developed a technology-friendly screening using Twistle as well as a paper screening form for those not wanting to use a cell phone.
To streamline the process, we are recommending that caregivers with the ability to do so complete this survey up to an hour in advance of your shift and prior to approaching a hospital screening location.
The process will vary slightly depending on your work location. Please see details below.
General Instructions for All Caregivers
Complete screening survey using Twistle on your cell phone within one hour before the start of your shift.
Open the camera on your phone to scan the QR code (below).
You’ll get a message at the top. Hit that message and it will automatically give you a text message that says COVID. Hit send and you will get a reply text to complete the survey.
OR text COVID to 833-453-0095.
- Twistle survey will open.
- Answer survey questions.
- If all responses are “no,” you will receive a green “all clear” message.
- Show your “all clear” to the screener on entry.
- If any answers are “yes,” will receive a red “do not enter” message. You will not be allowed to enter the building and will need to contact your manager to relay that you did not pass the screening. Your manager will direct you on next steps.
Christiana Hospital, Wilmington Hospital and Middletown Emergency Department
Entrances
To make the process as efficient as possible, we are limiting the access to these facilities to a few entrances. Caregivers should not use the main lobby entrances to report for work. Here are the newly designated, clearly marked entrances for screening and entry to the facility:
- Christiana Hospital – Ferguson Parking Lot entrance; employee entrance to the right of the main ED entrance; in the MAP I corridor for caregivers entering the hospital from Map 1 or Map 2 entrances.
- Wilmington Hospital – Gateway entrance.
- Middletown Emergency Department – Delivery entrance.
Caregivers are required to show their Twistle or paper screening results to a screener stationed at the designated employee entrances.
ChristianaCare HomeHealth
Complete the screening questions through the Twistle survey and forward the “all clear” to your manager including your own name in the message. If necessary, you can complete a paper survey to submit to your manager.
Outpatient, Administrative and All Other Service Locations
(such as Avenue North, Concord Health Center, PMRI, Ambulatory Testing/Diagnostic sites, Finance, etc.)
Complete the screening questions through the Twistle survey and forward the “all clear” to your manager including your own name in the message. If necessary, you can complete a paper survey to submit to your manager.
We encourage caregivers to use the Twistle screening process.
If you are not able to use Twistle, please use the paper form attached in this email. If you cannot bring it with you, a copy will be provided for you at the entrance.
Paper form screening process for all locations
- Complete the paper form prior to arrival for your shift, if possible.
- If you reply “no” to all questions, submit the paper form to your manager.
- If you reply “yes” to any questions, call your manager who will direct you on next steps.
Even with screening as an added layer of protection, it is vital that all caregivers remain compliant with hand hygiene, PPE and social distancing guidelines to prevent the spread of COVID-19.
Thank you for your patience and partnership as we implement this important new safety tool.
Sharon Kurfuerst, Ed.D., OTR/L, FACHE, FAOTA
Chief Operating Officer
 Loading...
Loading...
Covid Update 4/2
 Loading...
Loading...
Methadone
Methadone will be available through the OR pharmacy and only at Christiana Hospital. Attached is a one pager put together by Dr. Powell.
The methadone will be dispensed by pharmacy after an order is entered in Powerchart for a specific patient. Pick one of the IV injectable orders (search “methadone” for list)
You will receive a syringe with 20 mg. Use what you think you need and discard the rest with witnessed waste.
Methadone comes to pharmacy as a multidose vial. Once the vial is opened by pharmacy, it is good for 28 days. The syringe you receive is good for thirty hours. That is why the accudose is not stocked with a supply of syringes.
The primary indication for our use is complex spine surgery. Assuming elective surgery really does drop staring next week, we may not need it. Please don’t use methadone just to try it on a case next week since that starts the clock ticking on an entire vial of drug. However, should you have a good reason to use it, please do.
Questions and ideas back to me.
Mark Schneider MD, MBA
Director of Applied Innovation
Chair, Department of Anesthesiology
(o) 302-733-2676
(cell) 302-388-5211
Covid update April 1
Attached is the update for April 1. It contains a link to the new Covid-19 tracking dashboard at ChristianaCare. Updated every four hours, this live dashboard shows disposition of Covid patients in the two hospitals, number on ventilators and other interesting information. It is open to anyone with an 800 or 900 number. When you click to open, log in with your usual Powerchart credentials. You will probably need to be on the hospital network or logged in securely using two factor authentication from home. I have not tested that aspect.
The surge response plans referenced in the document are clipped in below. This shows the sequence of space utilization planned for ChristianaCare as the number of positive cases increases.
 Loading...
Loading...
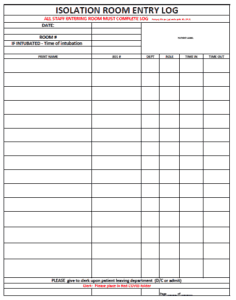
Covid Isolation Room Entry Log


Fentanyl, Sufentanil and Methadone at Christiana Hospital
In an effort to conserve supplies of fentanyl, one of the drugs currently experiencing supply chain interruptions, we are making sufentanil and methadone available for use in the OR. The use is restricted to Christina Hospital only at this time due to DEA licensing issues at the hospital level.
Sufentanil
Attached is a handy one pager developed by Dr. Cisler (thank you Sophia!) that explains the proper use of sufentanil. Please review it before using the drug. Sufentanil is being placed in the Omnicell machines at Christiana Hospital only . As you review the material and reacquaint yourself with its use, please send helpful hints, suggestions, corrections etc. to Dr. Cisler and myself.
Methadone
There is a limited supply of IV methadone in the system with scant to no availability from wholesalers. Dr. Powell will circulate suggested dosing for cases like complex spine. The methadone will be dispensed from pharmacy on a per patient basis as 20 mg in a syringe.. You must order it through powerchart, pharmacy then will pull a patient labelled syringe of the drug from their multidose vial. We are working out the mechanics as we speak, please be tolerant of initial glitches in the system.
Cost
Although costs really aren’t a factor right now, I know some people will be curious. Here is the breakdown of pharmacy costs.
Fentanyl
2ml = $0.53 per vial
5ml = $0.62 per vial
Sufentanil
2ml = $3.70
5ml = $8.00
Methadone
$33 per 20 mg dose.
 Loading...
Loading...
Trauma Alert and Code Response During Pandemic 2020
Updating Trauma response policy to limit providers in the room to conserve PPE etc. They are asking us to be present but to remain outside the trauma room and only enter when the code leader determines it is appropriate.
I assume there will be some unanticipated outcomes that will require adjustment of the policy, please filter those back to Dr Caruso.
Thank you.
Director of Applied Innovation
Chair, Department of Anesthesiology
(o) 302-733-2676
(cell) 302-388-5211
Covid-19 Update 3/30/20
 Loading...
Loading...
Out of state vehicles may be stopped by DE police as FYI
This article states that clearly out of state workers in health care are not impacted but police may stop vehicles with out of state tags to check them Just a heads up for all so no one has an anxiety attack!
Concise COVID Correspondence
Minimal updates today to hopefully decrease information overload! If you come across an area of uncertainty, there may very well be a plan in place, but every detail of every area is not being put into emails, or people will hate me. Dr. Schneider, Dr. Siry, Dr. Makai, Jen Bingnear, Will Arocho, Barb Evans, and myself are able to answer specific questions as they arise. Please do not hesitate to ask.
- N95 are now being utilized for 7 shifts of working. There are no specific manufacturer guidelines on duration of filtration. These have come from CCHS. Unofficial articles can be found online that address excellent filtration capacity for this duration of use as long as the mask is not soiled, and the mask fit continues to conform to the face.
- N95s remain in the intubation boxes to be utilized as replacements for PPE discarded after COVID+ intubations.
- Case bags have been created for the COVID+ cart to decrease use of items in the drawers as needed. You will notice paper tape on the drawers of the cart to alert the tech as to which drawers’ contents are contaminated after the drawer is opened. The bags have the essentials for either a GLMA or GETA case. Please ask the tech for the appropriate COVID+ case bag when requesting the COVID+ cart. Additional items that may be used are located in the COVID+ cart. Ideally the cart will not need to be opened during basic cases with the bags provided. This idea came from multiple staff members to use only the necessary equipment in these cases to avoid waste and contamination.
- Of note there is a McGrath 4 Blade and a 7.5ETT in the GETA bag. These items are compatible with GETA in most patients, even if not representing every provider’s ideal setup.
- You may call for in-line suction as needed, and the tech can pass it into the room.
- An alternative technique for removing your N95 was posted online by a CRNA and can be seen on the following link. COVID+ times call for Tupperware measures. https://www.facebook.com/Matt.Tom/videos/10103219262234777/
- Blue surgical hoods are in the anesthesia office near the intubation boxes if desired to protect the foam and strap of the face shield when going to the floor to do a COVID intubation. Be cautious to tie this behind your head so as to not contaminate yourself.
- Towels have been placed in the Main OR Call Suite Bathroom for provider use as needed to shower. TY Barb Evans for this care package
Please keep supporting each other and bringing on the good ideas. Enjoy your weekend!
Tara Hafycz, CRNA
Department of Anesthesiology
Clinical Coordinator, Christiana Main Operating Room
COVID Update 3/26/20
 Loading...
Loading...
PPE and COVID guidelines for the Main OR at Christiana
Please read these points carefully. They are meant to help guide utilization of PPE, staff, and resources in the time of this pandemic. Clinical decision-making always allows for variance as needed. Your patience in recognizing the dynamic nature of this disease is paramount. Guidelines are being designed expeditiously as new information is made available, with the intent of protecting providers and patients, while preserving supplies in a high-demand market. Things are changing as fast as we can write them. We appreciate the input of staff and I am AMAZED at the clear-thinking and problem-solving that has come from so many of our providers in creating these guidelines. Dr. Schneider continues to persistently advocate for our needs, and those of our patients. Many strides have been made due to his tireless efforts.
Thank you all for your work and support for our patients and each other.
All full face shields and N95s are on allocation from the department.
- Face shields should be wiped between cases with a PDI wipe. The OR provided them to our staff with the guidance that they are to be used for the duration of the pandemic. If they become soiled, or are used in a COVID or COVID rule-out patient, they are to be discarded and new items should be obtained from Theresa in the anesthesia office.
- N95s should be used for 40h breathing use. Time in your fancy brown bag does not count. They should NEVER be wiped off. If they become soiled, or are used in a COVID or COVID rule-out patients, they are to be discarded and new items should be obtained from Theresa in the anesthesia office.
- For masking purposes please consider all LMA cases in the same category as intubations.
- MAC cases should utilize contact and droplet precautions for masking purposes, unless converted to general. If converting to GA, please follow instructions for LMA placement/Intubations.
- Brown bags and face shields should be labelled. Please keep your brown bags in your pocket to reuse.
- Items should be kept in your locker when you are not working.
- New items will need to be obtained when going to a different site (Christiana vs. Wilmington). There are sign-out lists at each site.
- Regular surgical masks may be obtained by n95-INCOMPATIBLE staff members only via the OR staff member located near the pharmacy window at Christiana Main. You may not obtain a surgical mask if you have an N95. Regular surgical masks are to be worn for one shift unless they are soiled. They should be used in conjunction with a full face shield to prevent soiling.
- Additional N95 masks and face shields will be made available in a locked box in the office for weekend staff and off hours staff if they need new PPE due to soiling or COVID exposure. There will be a sign-out sheet located in the box to track the items removed. The locked box will be located on top of the filing cabinet next to the Vocera cabinet.
- Staff who present to work for their first encounter on the weekend at Christiana will find their N95 and face shield in the locked box in the anesthesia office. Theresa will contact staff working call at Wilmington to notify them where they will obtain their PPE supplies.
- Staff who are N95-INCOMPATIBLE will not be used for EGDs with open airways, ECTs, Bronchs, Trachs, or other aerosolizing procedures including to intubate or extubate patients, as PAPR supplies are not reliably available. These staff will utilize other providers for their intubations and extubations. We are working to ensure that pairings are not such that both the anesthesiologist and CRNA are in the N95-INCOMPATIBLE group.
- OR staff have been directed to follow the instructions of anesthesia staff regarding where to be during intubation and extubation. The ideal circumstances would allow for the surgical tech to stay as far away as possible during these events. The circulator, at your discretion, may also stay as far away as possible or immediately outside the door. They must remain immediately available to call ANESTHESIA STAT in such an emergency.
- For COVID or COVID rule-out patients:
- A COVID cart has been designed for use in known COVID or COVID rule-out patients. When a patient is assigned to your OR that has a COVID or COVID rule-out diagnosis, please call the tech to remove the current anesthesia cart, and replace it with the COVID cart.
- You will still need to obtain your drugs from pharmacy per normal fashion.
- There is a protocol for returning a pharmacy tray from a COVID or COVID rule-out patient. In the top drawer of the anesthesia cart there is a tray wrapper, label and instructions to follow. These must be completed.
- Please use contact precautions gowns for COVID and COVID rule-out patients.
- Please limit unnecessary staff in COVID rooms.
Tara Hafycz, CRNA
Department of Anesthesiology
Clinical Coordinator, Christiana Main Operating Room
Anesthesia N95 use for all intubations and aerosol generating procedures- WILMINGTON
Wilmington OR will be following the same process outlined by Dr. Schneider in last night’s email. Please see Wendy Glasgow in the Wilmington anesthesia workroom to obtain an N95 mask. One mask should be obtained per site and not be transported from site to site. On weekends, you will be contacted and allocated an N95 mask.
Please include ECT procedures in the list of procedures that should be performed with anesthesia staff wearing an N95 mask.
OR 2 is being set up as a Covid 19 room- Should Wilmington OR receive a Covid 19 patient who needs surgery, the surgery will be performed in OR 2. This room is set up with only essential supplies and closets are zip tied to prevent doors from being opened.
Thanks to everyone for your flexibility and understanding as PPE allocation is fluid and resources are changing on an hourly/daily basis.
Stacey Fletcher, CRNA, MSN
Clinical Coordinator
Department of Anesthesiology
Wilmington Operating Room
Cell- 302 528 3048
 Loading...
Loading...
Anesthesia N95 use for all intubations and aerosol generating procedures
Please see important change in practice starting Wed at 7 AM. Important to note that we need to preserve the N95s as long as possible – our supply is tenuous.
Mark Schneider MD, MBA
Director of Applied Innovation
Chair, Department of Anesthesiology
(o) 302-733-2676
(cell) 302-388-5211
 Loading...
Loading...
Albuterol Multi Dose Inhalers
Will be removed from the anesthesia drug trays. They will still be available in the OR pharmacies.
They are on backorder due to production issues int eh sully chain and from the move away from nebulizer treatments for Covid possible cases and use of MDI instead.
Mark Schneider MD, MBA
Director of Applied Innovation
Chair, Department of Anesthesiology
(o) 302-733-2676
(cell) 302-388-5211
COVID Update 3/23/20
 Loading...
Loading...
Conversion from airborne to contact droplet isolation and transport of patients
A recent case in the Christiana OR has highlighted some challenges and misunderstandings as to how to isolate and then transport patients.
- While it is appropriate to use airborne isolation for intubation or airway manipulation in suspected or test positive cases of Covid -19, it is policy to switch to contact droplet protection after one hour assuming the patient remains intubated. Anesthesia personnel may maintain N 95/PAPR protection after starting with the patient but should convert to contact/droplet if they leave the room after an hour and then return.
- When transporting the patient , it is important to think through conversion to contact droplet isolation so that, as the patient leaves the OR, staff still in airborne PPE can doff their current (presumably contaminated) PPE and change into clean contact/droplet. Arrange help for this process.
- Do not transport patients though the hall with airborne precautions. If they are intubated, used contact /droplet with a filter on the ambu bag.
- Once you drop the patient at their destination, please remove your isolation gown, doff your mask and eye protection and wash your hands. Right there outside the patients’ room. Please do not walk back through the hallways with your (presumably contaminated) PPE. You are more likely to infect yourself or someone else if you do not doff the PPE appropriately.
Happy to answer questions and receive comments, please e mail me directly.
Mark Schneider MD, MBA
Director of Applied Innovation
Chair, Department of Anesthesiology
(o) 302-733-2676
(cell) 302-388-5211
Mandatory Masking for Caregivers and Visitors- Effective March 23 at 3pm
Dear Caregivers:
Your safety is our top priority. To protect our caregivers and patients as community spread of coronavirus COVID-19 increases, we are requiring all visitors at ChristianaCare facilities to wear a surgical mask at all times, effective Monday, March 23, at 3 pm.
Additionally, we are requiring all caregivers to wear a mask when in a patient care unit in a hospital or emergency department, or in a patient care area in one of our outpatient practices. The required mask would be a surgical mask not an N95 or a respirator.
Caregivers are not required to wear a mask when not in patient care areas.
To ensure that we are using resources wisely and effectively, and to continue to maintain the supply needed for all caregivers, please use only one mask over multiple days/shifts, and replace it only when used for patients in isolation or when clinically indicated, or soiled or damaged.
If you have any questions about this policy, please address them to the COVID19info@christianacare.org e-mail address.
Yours in service,
Sharon Kurfuerst, Ed.D., OTR/L, FAOTA, FACHE, FABC
System Chief Operating Officer
